Double donor surgery on Crete saves lives
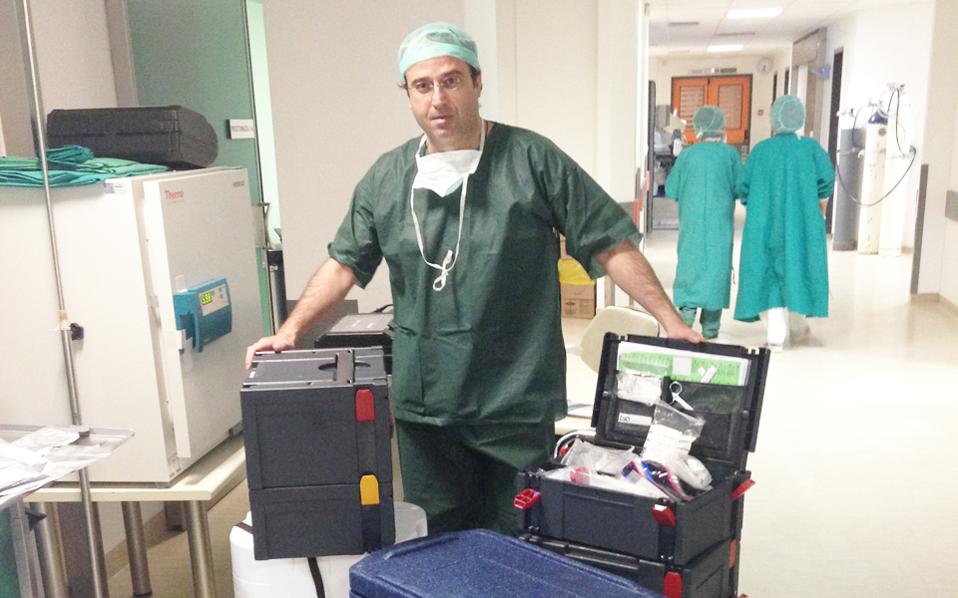
“Tonight, the heart of the organ donation system is beating in Iraklio, Crete. For the first time in Greece, a hospital is harvesting multiple organs from two donors at once. Countless tests, continuous communication of clinical information to the Hellenic Transplant Organization (EOM) and transplant units, and, more importantly, a sense of responsibility and sensitivity toward the donors’ families. The ORs are open and the staff is on alert. Over six transplant teams from the Evangelismos Hospital in Athens, the Ippocrateio in Thessaloniki, from hospitals in Italy and Germany and of course Iraklio will meet tonight in the operating theaters of Iraklio’s Venizeleio Hospital to build bridges of life. All of this has been made possible thanks to the superhuman efforts of doctors, critical care physicians, surgeons, anesthesiologists, transplant coordinators and nurses, to set up and succeed in such a demanding operation, in the framework of a system walking a tight rope.”
It was about 9 p.m. on Tuesday, January 12, when Iouli Menoudaki, supervisor of the EOM coordination center, made the above post on Facebook, describing the historical achievement. For the first time in the country’s medical history, a hospital, the Venizeleio on Crete, was conducting simultaneous organ transplants from two deceased donors.
The operation started in the morning, when EOM was informed by the Venizeleio’s ICU that they had two patients – a 58-year-old woman from the island of Kos and a 51-year-old man from Crete – who were brain dead and whose families had agreed to donating their organs.
“There was no room for delay,” Menoudaki told Kathimerini. “We could have had the surgeries over two consecutive days but the families wanted the bodies as they had already planned the funerals, so the two surgeries had to be held simultaneously. Once we were informed in the morning, we started getting the medical data on the organs’ function and began calling up the hospitals – the Onassis Cardiac Surgery Center for the heart, the Ippocrateio for the liver etc – and arranged for all the teams to travel to Crete for the retrieval.
“We don’t do lung transplants in Greece, so we got in touch with a team from Hanover, while for the second liver a team came from Bologna to take delivery of it. Teams from Athens’s Laiko, Evangelismos and Ippocrateio came to Crete for the four kidneys.”
The Venizeleio was on high alert. “The director, the anesthesiologists and surgeons went there that night to open the operating theaters. Even the driver spent all night going back and forth from the airport, transporting the teams of doctors and the organs,” said Menoudaki, adding that even the city airport stayed open beyond its regular hours.
After returning from Crete in the early hours of the following day, Dr Vassilis Drakopoulos from Evangelismos was supervising the next stage of the process.
“It is just as important to place the transplant properly as it is to remove them,” he told Kathimerini. “The donors made an amazing gift; a second chance at life. Because for someone suffering from kidney disease and having to undergo dialysis, a transplant is a gift of life.”
“It is the sweetest phone call when the coordinating teams tells you that a compatible donor has been found. You’re overjoyed, but then immediately you think that this means someone died.” Dimitris Magginas is 55 and spent 25 months waiting for a heart transplant, having to carry around a bulky power source for his artificial heart. He was diagnosed with heart disease in 2007. Finally, thanks to the vigilance of the doctors at the Onassis Cardiac Surgery Center and above all to the family of a 28-year-old called Nikolas who found the strength to donate his organs, Magginas has a new lease on life.
“The clock starts ticking from the moment you are diagnosed,” he said. “You wait. You don’t wait for someone to die, you just wait.”
Magginas considers himself lucky; some have to wait three years for a transplant and others are unable to enjoy even the limited freedom that he did.
“You keep your phone on all the time, 24/7. I got two calls. The first time, the coordinator told me a donor had been found but warned me that the organ may not be viable. That is what happened. The second time, it was a match. Nikolas was healthy and strong, and his parents are even stronger,” Magginas said.
Magginas and Nikolas’s parents are like family today after Magginas requested to meet them, “to say thank you.” They also wanted to meet the person who had their son’s heart.
“We are still in touch. They are part of my life and they treat me like their child,” said Magginas. “These people showed enormous altruism and love for their fellow man at the most difficult time of their lives. It is priceless. To all those who make the huge decision and who give a second chance to strangers, the least we can do is say thank you.”
Nikolas’s family hail from Crete, which, together with northern Greece, has the highest rate of organ donations in the country.
“Greeks are sensitive to the issue but they lack education and awareness,” said Magginas, who today serves as president of the Panhellenic Synechizo Association of Heart and Lung Transplants.
“The state needs to address the problem. I have been at the association for three and a half years and I have never spoken to a minister, a deputy minister or anyone else who is interested in doing something. Life cannot be calculated in money and even if if it could, they would see that it’s cheaper to do a transplant than all the other measures that are taken.”
Why is Greece a laggard in transplants? Is it a matter of social acceptance or a lack of political will? Does the crisis play a role? Kathimerini posed these questions to the president of EOM, Andreas Karabinis, professor of emergency medicine at the University of Athens and coordinating director of the Onassis Cardiac Surgery Center’s intensive care unit.
“To begin with, the most important thing is for society to acknowledge that organ transplants were one of the greatest breakthroughs in 20th century medicine. People with no hope, anchored to machines, now survive and enjoy a good quality of life thanks to transplants. This axiom needs to be accepted by society and it hasn’t. Recent statistics, such as those published by Eurobarometer, show that 50 percent of the population does not believe in transplants because it doesn’t trust the healthcare system.”
According to Karabinis, education is the way forward.
“The second problem is the shortage of ICU beds. When you don’t have enough for the living, how can you possibly keep a dead donor in the unit? The third obstacle, unfortunately, is that there is little education among doctors about transplants. Nevertheless, there are pockets of people inside and outside hospitals who believe in transplants and this is how we have been able to do them so far.”
The crisis, said Karabinis, has contributed to people’s reluctance to consider organ donation but is not a good enough excuse. “Paradoxically, other countries going through similar crises, like Spain, Portugal and Croatia, have not seen a drop in the number of donors and transplants. Nor is it purely a cultural issue. Even sadder is the fact that Croatia, with a population of 4.5 million, earmarks 1.4 million euros a year for transplants. EOM gets 280,000 euros a year, a ridiculous amount.”
Given these facts, a recent initiative by the Onassis Foundation to donate 100,000 euros to EOM for educational seminars for doctors and nurses was more than welcome.
Broken system
“These things are done in Greece out of our good will, because we believe we’re helping a good cause. All of this should be automatic, but it isn’t,” said one of the nurses who took part in the Crete operation, expressing her frustration and also some bitterness. It is painful, she said, to watch people die and their organs being lost because “the system” doesn’t work.
According to experts’ estimates, Greece has the potential to have 200 donors and over 1,000 transplants a year. Yet in 2015, just 91 transplants were achieved from 39 donors, making it the worst year to date (2008 was among the best with 266 transplants from 98 donors). The rates for organ donation per million of the population elsewhere in the European Union range from 17 to 25 donors, whereas in Greece the figure is at 6.5.
People involved in the issue say that one of the main problems is the absence of a reliable system to identify donors. Also, in Greece, what transplants are carried out are usually thanks to certain ICU doctors who take it upon themselves to inform EOM when a possible donor is declared clinically dead. However, a single organ donation can mean anything from 12 to 24 hours of additional work for the doctor, which is not covered by the hospital. That means potential donors are not declared because doctors are reluctant to take on the burden of the job without any remuneration. If the patient’s family is particularly persistent, an ICU doctor may agree but that will mean neglecting other duties as he or she will not be relieved from their regular duties. The sorry state of the system results in the following paradox: It is estimated that as much as 60 percent of all organ donations are achieved because the family has insisted.
One doctor who spoke to Kathimerini said that many donors are lost before they even reach the emergency room. “We don’t have enough beds in the ICU for patients who are still alive; we certainly can’t find enough for the dead,” he said. It is noted that the transplant process requires the donor to spend several hours in the ICU.
In many other countries, hospitals have special budgets to support a network of specialized emergency medicine doctors whose duty is not just to save their patients but also to identify potential donors and put the process into motion. Depending on the system, funding of between 5,000 and 20,000 euros is available in each case to pay the coordinating doctors, the ICU and the donor’s hospital care for the donor.
It is not just awareness of the relief that transplants can bring to suffering patients; there are also sizable potential economic rewards. For example, dialysis for each of the 11,000 kidney disease patients in Greece costs their respective healthcare provider around 40,000 euros a year, while the cost for the 50 patients who receive transplants abroad (for lack of a donor in Greece) comes to around 10 million euros a year. If Greece could get 200 donors a years, this would mean 240-300 kidney transplants, which would save some 6.7 million euros a year in dialysis alone.
But this is the country that allowed the EOM to be left with just one coordinator over the course of 24 hours on one summer day. According to EOM, it needs a staff of 24 people, eight of whom should be working as coordinators. Today it has just three full-time transplant coordinators and another 18 who have been assigned from other state services to cover the shifts over the 24-hour period.